Diabetic Retinopathy
The eye and diabetes
Anatomy of the eye and vision
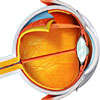 | The eye is the organ that allows us to see. The eyeball itself is a sphere spanning approximately 24 mm in diameter. It is suspended in the bony socket by muscles controlling its movements, and is partially cushioned by a thick layer of fatty tissue that protects it during movement within the skull. |
For more information, see The Eye and Vision.
Visual field testing
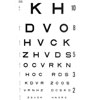 | Eye examination, also known as visual field testing, is the process of having the eyes examined for visual field defects or for monitoring changes in vision. Having the eyes examined regularly is the best way to detect vision changes and ensure that the conditions underlying changes in vision are diagnosed early. |
For more information, see Eye Examinations (Visual Field Testing).
Diabetes mellitus type 1
 | Type 1 diabetes mellitus is a chronic metabolic syndrome defined by an inability to produce insulin, a hormone which lowers blood sugar. It is predominantly a disease of the young, usually developing before 20 years of age. |
For more information, see Diabetes Mellitus Type 1 (Insulin Dependent, Juvenile Onset).
Diabetes mellitus type 2
 | Type 2 diabetes mellitus is defined by resistance to the hormone, insulin. This leads to inappropriate hyperglycaemia (increased blood sugar levels) and deranged metabolism of carbohydrate, fats and proteins. Rates are increasing, presumably due to the ageing population and increased rates of obesity. |
For more information, see Diabetes Mellitus Type 2 (Non-Insulin Dependent, Mature Age Onset).
Diabetic retinopathy
Diabetes and eye diseases
 | Diabetes is common, chronic condition that affects the body’s ability to control sugar levels. This can be due to autoimmune damage to the pancreas (Type 1 diabetes), or due to decreased effects of insulin due to poor diet, such as in the much more common Type 2 diabetes. Both these types of diabetes are associated with a wide range of complications, such as kidney disease or diabetic eye diseases. |
For more information, see Diabetes and Eye Diseases.
Diabetic retinopathy overview
 | Diabetic retinopathy, also called diabetic eye disease, refers to a group of eye diseases which affect individuals with type 1 and type 2 diabetes mellitus and occasionally individuals with pre-diabetes metabolic abnormalities (e.g. as in metabolic syndrome). |
For more information, Diabetic Retinopathy Overview.
Non-proliferative diabetic retinopathy
 | Non-proliferative diabetic retinopathy, previously called background retinopathy, is the earliest stage of diabetic eye disease. Microscopic changes occur in the blood vessels of the eye in non-proliferative disease; however, the changes typically do not produce symptoms and are not visible to the naked eye. |
For more information, see Diabetic Eye Disease: Non-Proliferative Diabetic Retinopathy.
Proliferative diabetic retinopathy
 | Proliferative diabetic retinopathy is an eye disease that affects diabetics. It occasionally also affects individuals with pre-diabetic metabolic abnormalities (e.g. metabolic syndrome). The condition is characterised by neovascularisation in the eye, and fibrous growth in the retina and surrounding vitreous fluid. It is a sight-threatening condition. |
For more information, see Diabetic Eye Disease: Proliferative Diabetic Retinopathy.
Diabetic macular oedema
 | Diabetic macular oedema is a sight-threatening eye condition. It is characterised by the leaking of blood from damaged vessels of the retina into the macula. Diabetic macular oedema affects diabetics with proliferative or non-proliferative diabetic retinopathy. The likelihood of developing diabetic macular oedema increases with the progression of non-proliferative diabetic retinopathy and is most likely when the condition progresses to proliferative retinopathy. |
For more information, see Diabetic Macular Oedema.
Ischaemic maculopathy
 | An individual with macular oedema also often has ischaemic maculopathy. Ischaemic maculopathy occurs in conjunction with macular oedema and may occur even when macular oedema is mild. Individuals with ischaemic maculopathy are at risk of severe vision loss. Treatments for the condition which can prevent vision loss have not yet been developed. |
For more information, see Ischaemic Maculopathy.
Dates
Tags
Created by:

 Login
Login














